This article draws from a recent webinar REDi Health hosted for rural providers across Oregon, centered on a question that has become increasingly urgent:
What does it actually take to turn Catalyst funding into measurable, lasting impact?
The arrival of Catalyst Awards through Oregon’s Request for Grant Funding Plan (RFGP) represents a meaningful opportunity. At the same time, it introduces a new level of accountability. Funding is no longer the endpoint. It is the starting point for demonstrating financial stability, operational improvement, and measurable outcomes tied to workforce and data modernization priorities.
For many organizations, the challenge is not a lack of effort or ambition, but a lack of clarity around where to begin.
Why This Matters Now
Moments like this tend to create urgency, and understandably so. Rural providers are being asked to move quickly, often while balancing day-to-day operational demands that have not eased.
The instinct is to act broadly. Invest in technology. Expand services. Address workforce shortages. Each of these areas is important. Yet when pursued simultaneously, without a clear sequence, they can become difficult to connect back to measurable outcomes. Progress may be made, but it becomes harder to demonstrate and even harder to sustain.
What distinguishes organizations that navigate this successfully is not the pace at which they act, but the order in which they act. The current environment does not simply reward activity. It rewards progress that can be clearly defined, measured, and defended over time.
A Structured Transformation Journey
Meaningful change in rural healthcare rarely occurs all at once. It follows a progression. One that begins with establishing a reliable foundation and builds toward long-term sustainability.
In the webinar, this progression was outlined as a multi-phase journey. It begins with stabilizing core elements. This includes ensuring data is accurate and integrated, identifying areas of financial leakage, and establishing baseline visibility into operations. From there, organizations move into improving performance through better analytics, reduced denials, and clearer insight into provider and system-level outcomes. Financial optimization follows, including contract alignment and reimbursement strategy. This leads into broader transformation with coordinated care models, operational efficiency, and sustained community impact.
This sequence typically unfolds over 18 to 24 months. It is not a rigid timeline, but a practical acknowledgment that each stage depends on the integrity of the one before it.
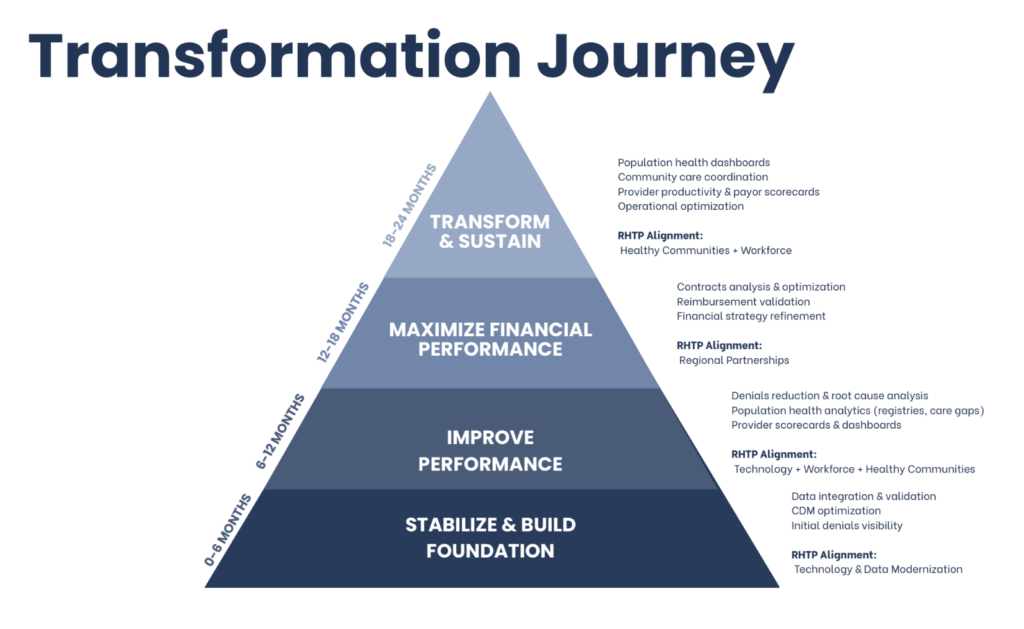
The value of this approach lies in its discipline. It reduces the risk of fragmented efforts and creates a pathway where each step contributes to measurable, cumulative progress.
A Practical Way to Begin
Understanding the full journey is important, but it does not resolve the immediate question of where to start.
What emerged clearly from the discussion is that effective starting points tend to share three characteristics. They align with funding priorities. They produce measurable outcomes. They can be executed within a structured, defined timeframe.
In practice, this means focusing less on large-scale transformation at the outset and more on targeted initiatives that create visibility and stability. These early efforts establish both the financial footing and the organizational confidence needed to support more complex work later on.
Early Impact: Financial Visibility and Revenue Integrity
Two areas in particular illustrate how this approach can take shape.
The first is Chargemaster optimization. While often viewed as a technical or administrative function, the Chargemaster plays a central role in revenue integrity. Over time, pricing can drift out of alignment with market benchmarks, and inconsistencies, especially across high-volume services, can lead to substantial but often unnoticed revenue loss.
A structured review, grounded in data and peer comparison, can correct these misalignments. In one example shared during the webinar, this process identified approximately $700,000 in gross charge opportunity without requiring additional patient volume or disruptive operational change.
The significance of this type of work extends beyond immediate financial gain. It establishes a more accurate and defensible financial baseline, which is essential for both internal decision-making and external reporting.
Denials management represents a complementary and equally important area of focus. While denials are frequently addressed at the individual claim level, this approach rarely captures the broader patterns that drive them.
A more effective starting point is visibility. By analyzing denial trends across payers, departments, and procedures, organizations can begin to understand not only the scale of the issue, but its underlying causes.
From there, the work shifts from remediation to prevention. Addressing upstream factors such as registration accuracy, documentation quality, and authorization workflows allows organizations to reduce denials at their source. Over time, this leads to more consistent performance and less reliance on reactive recovery efforts.
One example highlighted how improvements in registration processes not only reduced denial rates but also informed training that became part of staff onboarding, reinforcing those gains over the long term.
From Activity to Demonstrated Impact
What emerges from this moment is a shift in expectations. It is no longer sufficient to implement initiatives. Organizations must be able to demonstrate their impact in clear and defensible terms.
This requires a deliberate approach. One that prioritizes sequence, emphasizes measurable outcomes, and builds from a stable foundation toward broader transformation.
Catalyst funding creates the opportunity to make meaningful progress. Whether that progress can be sustained, and clearly demonstrated, will depend on how that opportunity is used.
In the end, the defining question will not be how quickly organizations acted, but how effectively they translated funding into results that endure.





