Committed to Progress
Blue Mountain Hospital’s leadership team is deeply committed to making steady, practical improvements that elevate the quality of care for their patients. At REDi Health, we’ve had the privilege of watching these changes unfold up close.
Denise Arthur in the business office and CFO Kent Turek set their sights on tackling a long-standing challenge: claims denials. They knew that they had a denials issue, but they didn’t know where to start. This project wasn’t their first step in that direction. In an earlier collaboration with REDi Health, using our Denials IQ tool, we worked together to bring greater transparency to their denial data and identify where to focus improvement efforts. That foundation gave the Blue Mountain team a clear, actionable starting point. As Denise explained:
We had a high-level view of the denials data, and that helped us drill down into a couple of projects that we could see would have the most impact.
Shining a Light on Denials
Building on the foundation laid with the Denials IQ tool, the Blue Mountain team—guided by Claire Adams, VP of Population Health at REDi Health, turned their attention to the denials contributing most significantly to revenue loss through REDi Health’s Denial’s Navigator. The tool organizes denial data in a way that supports meaningful, targeted decisions, breaking it down by denial code, payer, entry point (such as ED or inpatient), and specific claim details. This clarity helped the team identify where denials were most concentrated—and where to begin.
Using these insights, they formed three focused workgroups to address the biggest drivers of denials:
- Registration Denials
- External Medical Necessity
- Internal Medical Necessity
Among these, registration denials quickly emerged as a top priority. At the outset of the project, these denials alone were costing the hospital hundreds of thousands of dollars each year. Registration issues can stem from a variety of causes, including administrative missteps and coverage verification gaps. For example, a patient’s insurance might list their name as “John Doe,” but if the registration team enters “John H. Doe,” that seemingly small discrepancy can trigger a denial. Minor errors like this can result in the loss of reimbursement for a single high-cost emergency room visit—making registration an essential area to target for denial prevention.
While registration denials showed the most immediate ROI, the workgroups focused on medical necessity denials have also surfaced key learnings—such as gaps in documentation or inconsistencies in payer requirements—that the team is now addressing through provider training and internal audits.
As the work progressed, Blue Mountain Hospital also began seeing meaningful cultural and operational shifts. The Denials Navigator tool helped illuminate patterns by breaking down denials by payer and type, shining a light on where issues most often arose. This level of transparency, while powerful, can also feel vulnerable. As CFO Kent Turek acknowledged:
“Anytime you dig into data and scrutinize it, there’s fear of exposure. We’ve tried hard to show these are process improvement initiatives—not punitive. We’ve had to do focused work to help people understand that.”
We've tried hard to show these are process improvement initiatives--not punitive.
Kent Turek, CFO BMH
With this new visibility into where and why breakdowns were happening, Denise and her team could take precise, meaningful action. Rather than focusing on blame, the hospital’s leadership, alongside REDi Health, emphasized positive reinforcement, celebrating what staff were doing well and building training efforts around those strengths. The goal was sustainable improvement, rooted in shared accountability and aligned workflows.
And that’s exactly what began to take hold. With REDi Health’s ongoing support, the hospital embedded denial tracking into their everyday processes.
“We’ve created internal systems to track and trend denial information, plus very specific training based on the data,” Denise explained. “That training is now used to onboard registration staff—something we hadn’t anticipated but is now a huge benefit.”
These systems now serve as a foundation for ongoing progress, ensuring improvements are not just sustained but advanced over time.
That training is now used to onboard registration staff--something we hadn't anticipated but is now a huge benefit.
Denise Arthur, Business Office Manager
Turning Data into Dollars
Since partnering with REDi Health in 2023, Blue Mountain Hospital has seen a dramatic shift in its registration denial trends. In the
year leading up to this denials navigation work, the hospital faced a total of $1.2 million in registration denials—a significant financial challenge that demanded attention.
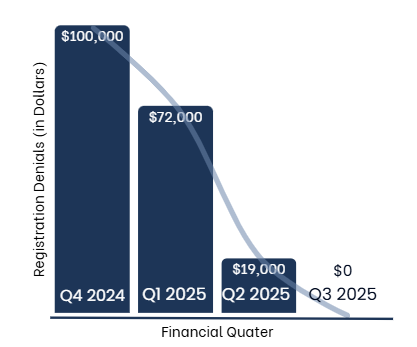
When Denise’s team began working with REDi Health, denials were climbing, peaking at $100,000 in Q4 2024. But meaningful changes quickly took hold: by Q1 2025, denials dropped to $72,000, then to $19,000 in Q2. Now, registration denials have fallen all the way to $0, a complete turnaround in just two quarters.
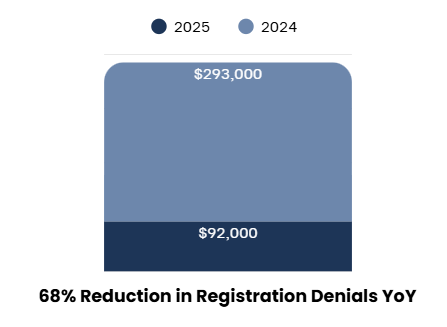
A closer look at year-over-year comparisons further highlights the impact: in Q1–Q2 of 2024, Blue Mountain recorded about $293,000 in registration denials. By the same period in 2025, that number had fallen to $92,000—a reduction of over $200,000, or approximately 68.6%.
These financial gains weren’t accidental; instead, they were the result of months of focused work identifying gaps, reworking processes, and building team capacity. Beyond denial dollars, this work has also reduced DNFB (Discharged, Not Final Billed) and shortened the time to bill, translating into faster payments. The billing office has seen a lighter workload as well, creating efficiencies that ripple upstream. Claire Adams, who led the project for REDi Health, reflected on the momentum they’ve built:
“We’re starting to see meaningful impact, especially on the registration side—small changes that compound over time.”
What Claire sees as the most impactful element of the work wasn’t just the dollar savings, but the clarity that came from data:
“We were able to give them a clear baseline—turning gut feelings into real dollar amounts. That visibility helped them mobilize, adjust processes, and see results.”
The results are already fueling reinvestment. With a strong business case rooted in the improved denial data, Denise successfully advocated for hiring an additional registration tech. What she presented to leadership wasn’t simply a case for cost recovery, but a clear argument for strengthening the hospital’s long-term capacity. It’s a clear example of how strategic insight can lead to tangible changes that make the hospital stronger for the community it serves.
That training is now used to onboard registration staff--something we hadn't anticipated but is now a huge benefit.
Denise Arthur, Business Office Manager
A Model for Rural Innovation
While it has taken intentional effort, the results are beginning to speak for themselves. As CFO Kent Turek observed,
“People start seeing data as an opportunity. It’s been a positive shift.”
That shift in mindset is empowering staff to act proactively. Denise shared how one team member, inspired by the project, took the initiative to build a resource list for providers to help avoid preventable denials—a small step with significant impact.
Targeted trainings now ensure that both current and future team members understand the correct protocols to prevent denials, especially those that are easily overlooked. As Denise put it, Blue Mountain is “proactively preventing denials now.”
That kind of forward-thinking mindset is exactly what rural hospitals need. While funding sources may remain uncertain, hospitals like Blue Mountain are showing that meaningful progress is still possible. At REDi Health, we’ve seen how initiatives like this—low-barrier, high-impact projects—can empower hospitals to take control of their financial future.
Kent offered thoughtful advice for other hospitals considering a partnership with REDi Health:
“Go into it with an open mindset. Even if you think your processes are great, REDi can help you uncover opportunities. Just give them access and let them explore. Every organization will discover something valuable.”
Go into it with an open mindset. Even if you think your processes are great, REDi can help you uncover opportunities.
Kent Turek, CFO
Blue Mountain’s success is proof that rural hospitals can innovate, thrive, and protect their communities—even when margins are tight. Their example lights the path forward for others navigating uncertainty with courage, clarity, and creativity.
About REDi Health
REDi Health helps small and rural hospitals make the most of their data by empowering staff and partnering to drive sustained improvement. Instead of introducing new technology, the focus is on maximizing the value of existing systems—building on past innovations with a hands-on, personalized approach. Supporting sustainable rural healthcare requires collaboration, and REDi Health is proud to be part of that journey.
Experience shows: life is better with data.






